How to Manage Dry Eyes in Air-Conditioned Environments During Summer
Learn effective strategies to prevent and manage dry eyes in air-conditioned spaces..
Read More
Saraswati Eye Care Centre is the most trusted and highest-rated eye hospital in Jind, Haryana — as reflected in our Google reviews and patient satisfaction. We take pride in being the first NABH-certified eye care hospital in District Jind, offering comprehensive, ethical, and technology-driven eye care services under one roof.
Founded by Dr. Rajesh Garg, a renowned anterior segment surgeon and expert in customized cataract surgery, the hospital has grown from a small clinic into a state-of-the-art super-speciality eye centre, serving thousands of patients with compassion and precision.
To provide world-class, affordable, and comprehensive eye care services to all, and to become a leading name in super-speciality ophthalmology across North India.

Founder & Chairman

Retina & Vitreous Specialist

Pediatric Ophthalmologist

Glaucoma Specialist

Anaesthesiologist
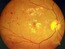
Vitrectomy for retinal detachments, epiretinal membrane, macular hole, vitreomacular...
Early detection and treatment are crucial for preserving vision in retinal conditions.
Read More...

Myopia clinic specializes in diagnosing, treating, and managing myopia, also known as nearsightedness
Read More..

Diagnosis and management of pediatric eye disorders like refractive error.
Read More...
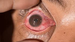
The Uveitis & Ocular Immunology Service provides multidisciplinary...
Read More...




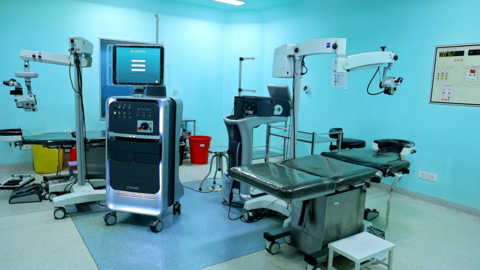






Explore our collection of informative and educational videos about eye care and treatments
Take a virtual tour of our state-of-the-art facility and meet our expert team
By Dr. Rajesh Garg
By Dr. Rajesh Garg

Learn effective strategies to prevent and manage dry eyes in air-conditioned spaces..
Read More
Understanding childhood myopia, its causes, early signs, and effective prevention methods...
Read More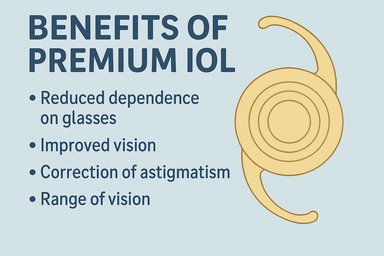
Explore the advantages of premium IOLs and determine if they're the right choice for your vision...
Read More
Comparing different anesthesia methods in cataract surgery and their safety profiles...
Read MoreBook your appointment today and take the first step towards clearer vision with our expert eye care services.
BOOK an appointment today to get expert advice and treatment to your eye problems.